 
The tip of the tongue may also impede the fusion of the palatal shelves, leading to cleft palate. The tongue continues to grow normally and is ultimately displaced backward, causing potential obstruction of the upper airway. This may be caused by multifetal gestation, uterine anomalies, or oligohydramnios. This theory proposes that external forces cause the fetal head to become flexed, compressing the mandible against the chest, rendering it unable to grow appropriately. This theory proposes a delay in the neuromuscular development of the tongue, which in turn does not stimulate the mandible to grow appropriately or palatal shelves to fuse. The glossoptosis, due to abnormal mandibular growth, ultimately leads to upper airway obstruction. If mandibular growth is abnormal, the tongue is not able to follow the normal trajectory of growth and blocks the closure of the palatal cleft in the 11th week of gestation. In the early first trimester, around the 7th week of gestation, the mandible typically grows ventrally and inferiorly. The following are common theories behind the hypoplastic mandibular growth. In PRS, micrognathia is the first abnormality that leads to glossoptosis and, ultimately, airway obstruction and/or a cleft palate. 
A syndrome, in contrast, is a set of anomalies that arise separately due to one underlying pathogenesis. Pierre Robin sequence (previously named Pierre Robin syndrome) is now correctly named a sequence because one initial malformation leads to a sequential chain of events causing the other anomalies. EpidemiologyĮpidemiological data is sparse, but available evidence suggests that PRS affects approximately 1 in 8,500 to 1 in 14,000 newborns a year. Clinical features include hypoplasia of zygomatic, maxillary, and mandibular bones, and anomalies of the temporomandibular joint (TMJ), cleft palate, and external ear. Treacher Collins syndrome has mutations in TCOF1, POLR1C, and POLR1D genes. Clinical features include long upper lip and philtrum, elongated face, slender digits, hypothyroidism, immune dysfunction, hearing loss, pulmonary atresia, ventricular septal defects (VSDs), and hypoplastic pulmonary arteries. Velocardiofacial syndrome is a 22q11 deletion syndrome or TBX1 gene resulting in abnormalities in heart, parathyroid, thymus, and facial development. Clinical features include flat midface, epicanthal folds, retinal detachments, cataracts, joint hypermobility, and sensorineural hearing loss, in addition to the typical signs of PRS. It is an autosomal dominant condition defined as a mutation of COL genes, affecting collagen formation. In one study, 47% of syndromic PRS patients were diagnosed with Stickler syndrome. Stickler syndrome is the most common syndrome associated with PRS. There have been 34 syndromes associated with syndromic PRS, the most common being Stickler syndrome. Alternatively, syndromic PRS has been recently reported to account for 60% of PRS. Some evidence suggests SOX9 or KCNJ2 mutations (on chromosome 17) may affect the development of facial structures and cartilage development, leading to PRS. Non-syndromic PRS has been associated with mutations on chromosomes 2, 4, 11, or 17. The etiology of PRS is typically separated into isolated and syndromic PRS. However, Pierre Robin first published a case of an infant with these characteristics in 1923. The sequence was first described in 1891. These findings may be part of a syndrome or isolated. It is commonly associated with cleft palate. Clinically, this results in a small, underdeveloped mandible that causes the base of the tongue to fall back into the throat and can ultimately lead to upper airway compromise. Pierre Robin sequence (PRS) is characterized by the clinical triad of micrognathia (mandibular hypoplasia), glossoptosis (downward displacement of the tongue), and upper airway obstruction. 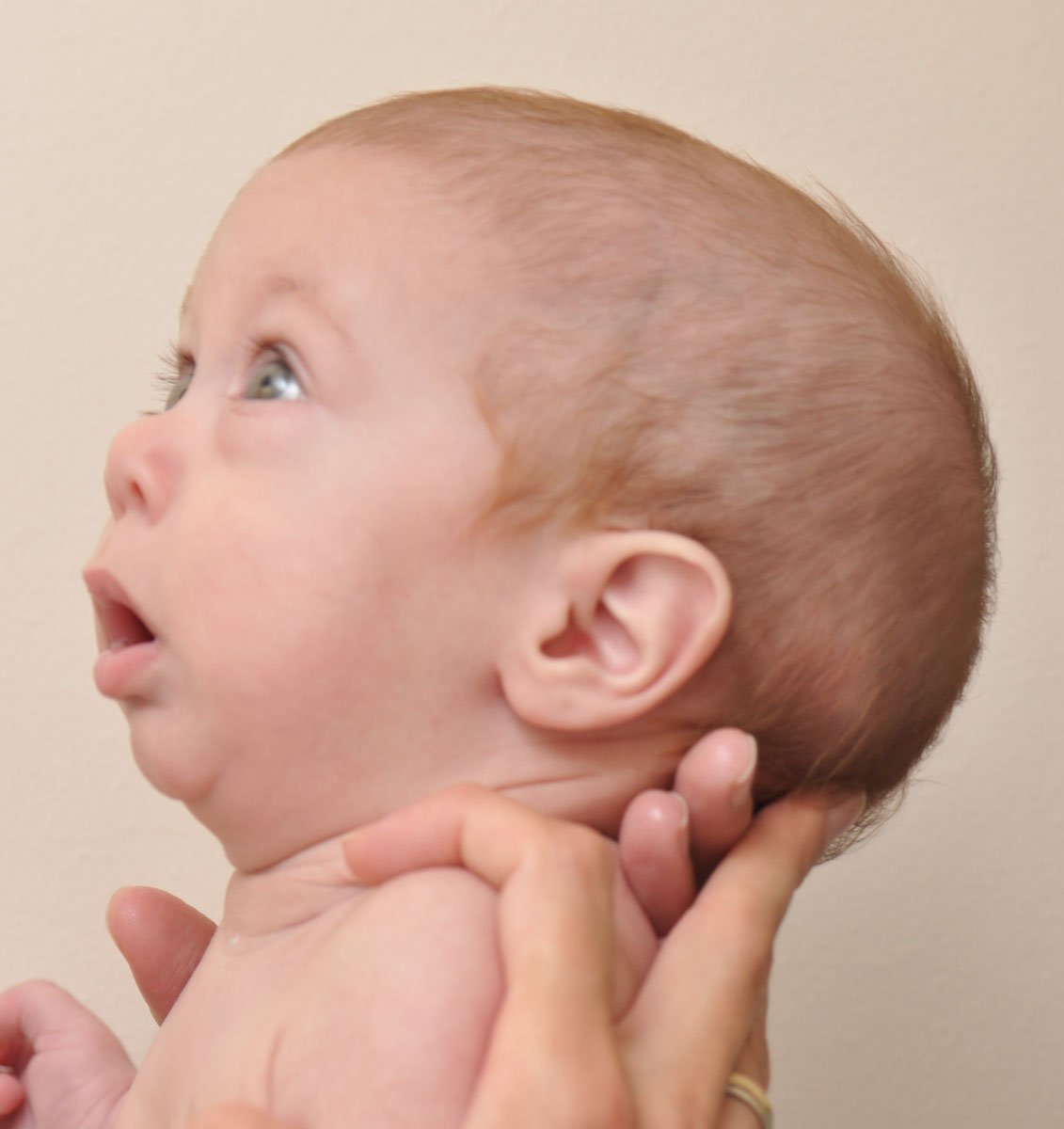
Review interprofessional team strategies for improving care coordination and communication during prenatal parental counseling of Pierre Robin sequence to enhance the care of patients with this condition.Outline the treatment considerations for patients with Pierre Robin sequence.Describe the classic physical exam findings associated with Pierre Robin sequence. 
Summarize the etiology of Pierre Robin sequence.This activity describes the evaluation and management of Pierre Robin sequence and reviews the role of the interprofessional team in managing patients with this condition. It is a clinical diagnosis that can range in severity and may be associated with genetic syndromes. Pierre Robin sequence is a constellation of micrognathia, glossoptosis, and upper airway obstruction. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
